Two of the most useful — and often overlooked — components of the nutrition physical exam are the tongue and fingernails. Together, abnormal findings can often be sourced to gut. In this blog, I’m presenting a case where tongue and nails were extremely useful in providing clear treatment direction. Next month, I’ll give some additional practice pearls for tongue diagnosis.
Last summer I blogged about the nail physical exam, “Fingernails: A window into your metabolic soul”.
Virtually EVERY nutrient deficiency can alter how our nails grow.
In my practice I most often see the impact of protein, mineral and B vitamin insufficiencies/deficiencies contributing to a range of nail abnormalities, including brittle (onychorrhexis), spooned (koilonychia), white-spotted (leukonychia) or lined/ridged nails (longitudinal or transverse). Note that we can also see certain conditions present with nail changes, such as the tell-tale pitting often found with (or preceding the onset of) psoriatic arthritis, but for this blog, I’m focusing specifically on nutrient-associated nail changes.
A young female vegan who presents with koilonychia is probably, but not always, iron deficient because she’s not consuming enough iron in her diet.
When I see nail abnormalities without any obvious cause, however, the logical question is WHY?
If an individual consumes a reasonably healthy diet, has no recent history of a significant illness, and has nail changes suggestive of mineral/protein/B vitamin deficiency, what’s causing this?
Nails take at least six months to grow out. So if the growth pattern involves the entire nail plate, we’re not looking at a sudden change. (And if it IS a newer change, you should see that reflected in the nail growth pattern. A detailed history should give you an idea of what happened to cause the nail growth alteration.)
Most often, I’m sourcing nail nutrient deficiencies back to something happening in the gut. Something is contributing to mal-digestion and/or malabsorption.
Now look at your patient’s tongue. Before jumping to an extensive laboratory work-up, we can generally get good clues as to what’s happening in the gut by looking at the tongue.
Janice was 42 years old when she first came to my practice. Her chief complaints included a 30-pound weight increase over the course of a year, significant fatigue, and gas and bloating after eating. She is a lifetime athlete, most recently a triathlete; but while she continued to push herself to train, she hadn’t competed over the last year due to her overwhelming fatigue.
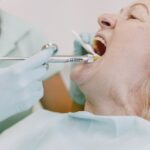
Janice. Baseline tongue image. Coating suggestive of dysbiosis/yeast overgrowth. Foods can discolor the tongue, most commonly coffee, so confirm that nothing has been recently consumed.
Janice. Baseline nails image. Brittle (onychorrhexis), with ragged cuticles (paronychia).
Given Janice’s nails, I suspected mineral deficiencies. Brittle nails are most often associated deficiency of iron, zinc, calcium or magnesium, although protein deficiency and hypothyroidism can cause brittle nails. We can also see brittle nails in folks with low stomach acid, probably due to hypochlorhydric-induced mineral malabsorption. Think about this with individuals on acid-blocking therapy of any kind.
(Pearl: Brittle nails can also parallel bone loss. Improvements in nails are seen with improvements in bone density. Not surprisingly, osteoporosis is a known side effect of chronic acid blocking therapy, aka hypochlorhydria.)
The coating on Janice’s tongue combined with gas and bloating after meals suggested hypochlorhydria, plus some kind of dysbiosis/SIBO, of bacterial and/or fungal origin. I suspected that poor digestion was therefore a likely cause of her mineral deficiency. And I also suspected her lifetime of athletics was a piece of the puzzle, too. Long term athletes are vulnerable to developing intestinal permeability, dysbiosis and nutrient deficiencies.
Janice. Baseline D-arabinitol was very elevated. D-arabinitol is a sugar alcohol produced specifically by candida species.
As shown in the figure above, Janice’s baseline D-arabinitol was very elevated confirming GI candidiasis. Other labs confirmed zinc and magnesium deficiency, mild functional hypothyroidism (TSH = 3.13) and adrenal fatigue. Her mean cell volume was functionally elevated at 94. She had elevated IgG antibodies to soy, wheat, egg and casein.
I prescribed Janice a low sugar Paleo style diet with an HCL titration. (For the titration, ~500mg betaine HCL capsules are used, starting with one and increasing at each main meal by one capsule, until a very slight warmth is felt in chest/epigastric region.) For the candidiasis, we used Oregano oil and a compounded sugar-free nystatin. I also gave her a high potency mineral supplement, B12, vitamin D, fish oil, adaptogen botanicals for adrenal support and ½ grain of Armour thyroid.
Janice responded well to treatment plan. She lost weight, her energy bounded back, her nail growth was strong, and her tongue improved. She returned to competing in triathlons, and won in her age group!
As I thought about writing a “tongue blog” this month, I checked in with Janice for an update. Here’s what she had to say:
My tongue is my best indicator of my nutrition and inside health. Too much sugar….white coating…..some type of reaction to food/spice…..scalloped edges. When I’m eating clean….[my tongue is] pink.
Follow-up D-arabinitol
Janice. Follow-up nails.
Janice. Follow-up tongue. No coating, but there is mild scalloping. I’ll talk about this finding in greater detail next month.
Related Blogs:
Dr. Fitzgerald is the lead author and editor of Case Studies in Integrative and Functional Medicine and is a contributing author to Laboratory Evaluations for Integrative and Functional Medicine and the Institute for Functional Medicine (IFM)’s Textbook for Functional Medicine. With the Helfgott Research Institute, Dr. Fitzgerald is actively engaged in clinical research on the DNA methylome using a diet and lifestyle intervention developed in her practice. The first publication from the study focuses on reversal of biological aging and was published 04-12-2021 in the journal Aging. She has published a consumer book titled Younger You as well as a companion cookbook, Better Broths and Healing Tonics and has an application-based Younger You Program, based on the study.
Dr. Fitzgerald is on the faculty at IFM, is an IFM Certified Practitioner and lectures globally on functional medicine. She runs a Functional Nutrition Residency program, and maintains a podcast series, New Frontiers in Functional Medicine and an active blog on her website, www.drkarafitzgerald.com. Her clinical practice is in Sandy Hook, Connecticut.
Around July of this year I noticed changes on my tongue that I know now is referred to as glossitis. I had been on a long term dose of Keflex for a UTI that was started April 5, 2019 (took for 3 consecutive months). I also started a troche on July 15, 2019 of combined estrogen and progesterone (I am 48 and going through menopause).
I am in the process of doing blood work to check for b vitamin deficiencies and celiac disease. My B12 has been checked and it is actually above where it should be. My iron and Thyroid look normal. My internist gave me a script for Diflucan and magic mouth wash that contains nystatin but neither are making a difference except the mouth wash eases the pain.
I’m not sure what to do at this point or how to figure out the culprit. Was it the long term use of the Keflex, hormonal changes…..
I have the same color tongue as the pic of Janice along with the red dots and fissures. I am not local to CT and have been researching as much as I can bc the doctors where I live do not really seem to have any answers.
Do you have any suggestions? Advice? Anything would be much appreciated.
This content was originally published here.
















![Period Exercise [Workout To Do During Period]](https://thehealthandwellnesscrier.com/wp-content/uploads/2023/03/Period-Exercise-Workout-To-Do-During-Period-768x432.jpg)
